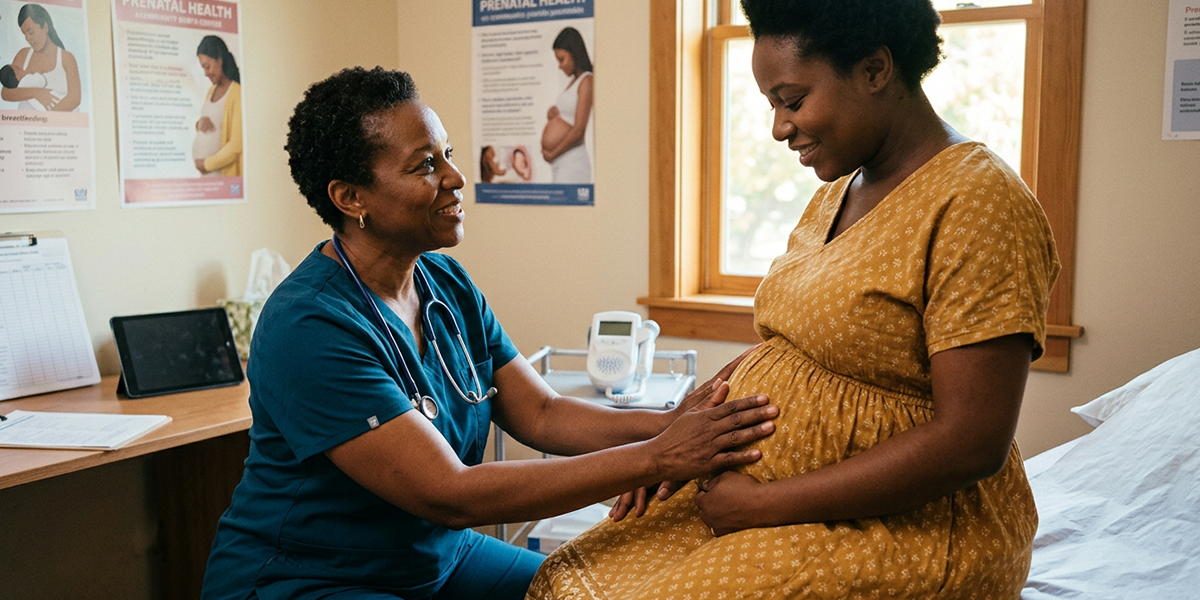
Rural Missouri is attempting to build a new maternal health infrastructure. The question is whether the workforce will be allowed to practice.
When the delivery department at Hedrick Medical Center in Chillicothe shut its doors, it did more than eliminate a service line. It removed a lifeline for women like Leigha Leppin, a mother of 11 in north-central Missouri who had experienced partial placental abruptions, a dangerous condition in which the placenta separates prematurely from the uterine wall, in two previous pregnancies. Those emergencies had been treated by obstetricians 20 minutes from her home. Now, her nearest option for delivery was Saint Luke’s Hospital of Kansas City, more than two hours away. “Our small hospital could probably do enough to save me. But that wasn’t just my goal. It was for both of us, too.” Leppin told the Columbia Missourian. “And so I honestly was just willing to risk it all to get us both someplace safe.”
Leppin’s experience is not unusual. It is, increasingly, the standard reality for pregnant women across rural Missouri.
More than half of Missouri’s 114 counties, 51.3%, qualify as maternity care deserts, meaning they have no hospital or birth center offering obstetric care and no obstetric clinician. That rate far exceeds the national average of 35% and continues to rise as obstetric units close. Missouri has lost 11 hospital obstetric units since 2009, seven of them in rural areas. As a result, nearly 18% of births in the state, roughly 12,900 per year, occur to parents living in counties with no local maternity care, according to the March of Dimes. Women in these counties have to travel 3.6 times further to reach a provider. A 2025 study in Obstetrics & Gynecology found that maternal mortality in desert counties runs 36% higher than in counties with full access. Nine of Missouri’s 10 counties with the highest infant mortality rates are rural.
Dr. Kelsey Davis-Humes sees the full scope of this crisis every day. As an osteopath in Scotland County in northeast Missouri, she provides primary care, delivers babies, provides pediatric and newborn care, covers inpatient hospital shifts, and visits the nursing home. “In general, you see more high-risk patients,” Davis-Humes told the Missouri Independent. “People are sicker, they’re more unhealthy, so we just see more patients that have more of these high-risk conditions during their pregnancy.”
Into this landscape comes one of the most significant federal investments in rural health in a generation. In December 2025, the Centers for Medicare and Medicaid Services announced $50 billion through the Rural Health Transformation Program. Missouri received $216 million for fiscal year 2026, while Kansas received $221 million. Across the country, maternal health quickly emerged as what analysts described as a “keystone issue,” exposing deeper weaknesses in rural health systems.
Missouri’s plan, called Transformation of Rural Community Health, or ToRCH Care, envisions seven regional coordinating networks and up to 30 community hubs spanning two to five counties each. The model repositions rural hospitals as anchors for integrated care, connecting physical health, behavioral health, and social services through a shared digital platform. Kirk Mathews, chief transformation officer for MO HealthNet, has pointed directly to maternal health as a priority, noting that addressing barriers such as transportation and nutrition for pregnant rural Medicaid enrollees could improve healthy birth weight rates and reduce costly NICU stays. Kansas is pursuing a parallel strategy through a $44 million Regional Partnership Grant Program, bringing together hospitals, clinics, and behavioral health providers in collaborative arrangements.
The architecture is promising. But it requires a workforce. And the workforce best positioned to staff these hubs– doulas and midwives– faces barriers that no amount of federal funding automatically resolves.
The Workforce Rural Maternity Care Depends On
The evidence base for doula care has never been stronger. A 2024 study in the “American Journal of Public Health” analyzing nearly a decade of Medicaid claims found that women who received doula care had a 47% lower risk of cesarean delivery and a 29% lower risk of preterm birth. They were 46% more likely to attend a postpartum checkup, which is critical given that the highest incidence of maternal deaths occurs 43 days to one year after delivery. A 2025 study in the “American Journal of Obstetrics & Gynecology” found three to four fewer preterm births for every 100 patients who received doula care, with effects consistent across race and insurance status. Research published in the journal “Birth” found Medicaid coverage of doula services could save states money, with one model estimating $58.4 million in annual savings and 3,288 fewer preterm births regionally.
Missouri took an important step when MO HealthNet began reimbursing doula services in October 2024, a victory driven in large part by the years-ong advocacy of Hakima Tafunzi Payne, co-founder and CEO of Uzazi Village in Kansas City, and Okunsola M. Amadou, founder and CEO Emeritus of Jamaa Birth Village in Ferguson. Together, they co-founded the Missouri Community Doula Council, which now oversees the statewide eligible doula directory and training infrastructure. The Missouri Doula Association works alongside the council to unite and support doulas across the state.
But reimbursement alone does not build a rural workforce. Amadou has worked to expand the pipeline, training additional midwives and planning birth center expansions. “We know that hospitals are overwhelmed. They’re understaffed. Providers in the hospital are exhausted, and doulas can only support so much,” Amadou told the Missouri Independent. “So we’re able to open a birthing center and also train additional midwives, additional Black midwives, in clinical care practices, and we can really help to advance maternal health.” In mid-Missouri, Erica Dickson founded the Mid-Missouri Black Doula Collective in Columbia and is expanding into rural communities, including Jefferson City, Boonville, and Sedalia. “We want to make sure we are covering more ground as far as being able to offer services in different places,” Dickson told COMO Magazine.
One partnership already operating in Missouri offers a working model of what ToRCH’s community hubs could look like if safety-net providers and community-based organizations align. Altruism Inc. opened The MaIH Center in rural Lexington in 2022, embedding doulas, midwives, and community health workers in Lafayette County to serve birthing people on Medicaid or without insurance. In June 2025, Altruism expanded by opening The MaIH Center at Sam Rodgers through a partnership with Samuel U. Rodgers Health Center, a federally qualified health center in Kansas City, co-locating nonclinical maternal support services alongside Sam Rodgers’ maternity care clinic at its Cabot Westside location. The partnership, believed to be the first of its kind in the Midwest, brings doula care, prenatal education, and mental health services under one roof alongside OB visits, WIC, and dental care. “When you talk about wraparound care, this partnership does that,” Tonia Wright, Altruism’s CEO, told KSHB.
The model matters because Missouri’s ToRCH framework explicitly allows federally qualified health centers to serve as community hub anchors in regions where hospitals have closed. Heidi Lucas, executive director of the Missouri Rural Health Association, told Stateline that in parts of the state where multiple rural hospitals have shuttered, “the FQHC is the only provider.” If the Altruism/Sam Rodgers model can be replicated through ToRCH’s regional networks, it would give rural communities without hospitals a pathway to integrated maternal care that pairs clinical services with the doula and midwifery workforce the evidence supports.
But scaling that model requires addressing the regulatory barriers that constrain it. Certified nurse-midwives attend roughly 30% of deliveries in rural hospitals nationally, according to the American College of Nurse-Midwives, and, for low-risk pregnancies, achieve outcomes comparable to or better than physician-led care. Missouri, however, requires certified nurse-midwives to maintain collaborative practice agreements with physicians, a requirement that becomes practically impossible in counties where no physicians practice. States granting midwives autonomous practice authority see 34% of their rural hospitals with midwives attending births, compared with 28% in states requiring physician agreements. Missouri also does not license or reimburse certified professional midwives through Medicaid, a category of provider trained specifically for community-based births that would align naturally with the hub model.
The broader policy environment adds another layer of uncertainty. The same legislation that created the $50 billion Rural Health Transformation Program embedded significant Medicaid cuts. The Health Forward Foundation has noted that the RHT’s funding covers only a fraction of the estimated $155 billion in cuts to rural health practitioners. Missouri’s Medicaid program stands to lose roughly $1.9 billion per year, money that currently pays for the pregnancies, deliveries, and postpartum coverage that more than 40% of Missouri births depend on.
The community hubs being built in Missouri and Kansas could mark a turning point for rural maternal health. The Altruism/Sam Rodgers partnership demonstrates what is possible when clinical safety-net providers and community-based maternal health organizations work together under one roof. But replicating that model statewide will require training pipelines into rural communities, scope-of-practice reforms that allow doulas and midwives to practice where physicians can’t be found, and the political will to prioritize maternal health not just in grant applications but in state law.
Rural Missouri is not short on need, nor on evidence. The ToRCH is lit. Whether it illuminates a path forward depends on what happens next.