Every year for nine years, gestational diabetes rates climbed. Not most years. Not in certain regions. Every single year, without exception.
Gestational diabetes rose every single year in the United States between 2016 and 2024, increasing 36% over that period, according to a Northwestern University Feinberg School of Medicine study published in “JAMA Internal Medicine.” The condition, which raises health risks for both mother and baby, climbed from 58 to 79 cases per 1,000 births.
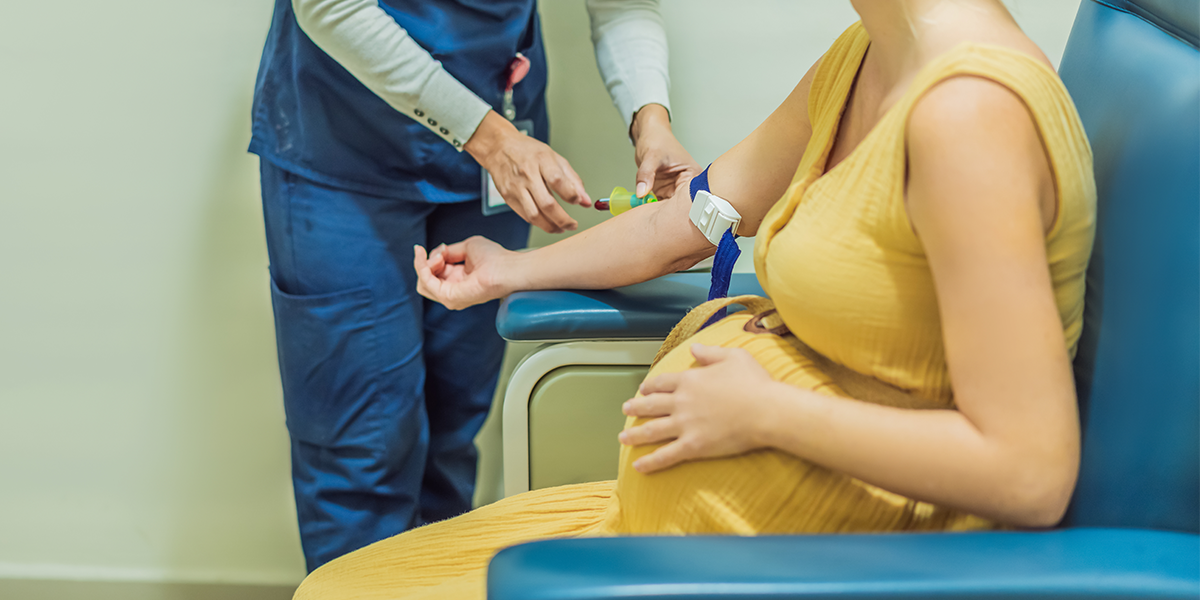
For pregnant women in Missouri and Kansas, those numbers represent more than statistics. They reflect the reality of managing a complex medical condition while navigating systems that were not designed to support them. Daily blood sugar testing. Weekly doctor visits. Work schedules that do not allow for frequent medical appointments. Rural areas where the nearest obstetrician may be an hour away.
“Gestational diabetes has been persistently increasing for more than 10 years, which means whatever we have been trying to do to address diabetes in pregnancy has not been working,” said Dr. Nilay Shah, senior author of the study and assistant professor of cardiology at Northwestern University Feinberg School of Medicine.
Before Pregnancy: The Coverage Problem
In Kansas, an estimated 39,000 people remain in a coverage gap created by the state’s decision not to expand Medicaid under the Affordable Care Act. These are primarily working adults who earn too much to qualify for traditional Medicaid but too little to afford marketplace insurance, even with subsidies. For women of childbearing age, this gap often means years without access to preventive care before becoming pregnant.
Missouri expanded Medicaid in 2021, extending coverage to approximately 275,000 residents, according to the Centers for Medicare and Medicaid Services. But that expansion came after more than a decade during which low-income Missouri women of childbearing age had limited access to routine health care. By the time pregnancy made them eligible for coverage, metabolic dysfunction often had gone undetected for years.
Research shows that children born to mothers with gestational diabetes face heightened risks for obesity, glucose intolerance, and cardiovascular disease throughout their lives. A 2025 review published in the journal “Life” found that maternal hyperglycemia leads to long-term metabolic changes in offspring through epigenetic modifications. Studies suggest that up to 20% of children born to mothers with gestational diabetes develop Type 2 diabetes or prediabetes by age 22, and they face a 29% higher risk of early-onset cardiovascular disease.
During Pregnancy: Geography as a Barrier
Once pregnant, women face a different obstacle: access to care. In Missouri, 41.7% of counties are classified as maternity care deserts, compared with 32.6% nationally, according to March of Dimes data. The state has lost 11 obstetric units since 2009, including seven in rural areas, according to an August 2025 report by Missouri Independent.
Kansas mirrors this trend. The state lost 17 rural obstetric units between 2011 and 2023, according to the March of Dimes. A 2025 Chartis Center report found that 47% of rural hospitals in Kansas are financially vulnerable.
Women living in maternity care deserts travel 3.6 times farther for prenatal care than those in adequately served areas, March of Dimes research shows. For women with gestational diabetes, distance compounds an already intensive care regimen.
Managing gestational diabetes requires checking blood glucose levels four times daily, once fasting and after each meal, according to clinical guidelines. Women typically need weekly prenatal visits to review glucose logs, along with appointments with nutritionists and diabetes educators. Those requiring insulin need additional visits for dose adjustments. Beginning at 32 weeks, fetal monitoring becomes necessary, often once or twice weekly.
Research on rural gestational diabetes care shows that transportation costs and distance are major barriers to diagnosis and treatment. Women in rural areas must travel regularly under difficult conditions during advanced pregnancy, often requiring an escort, which adds to both cost and complexity.
The time demands extend beyond medical appointments. Neither Missouri nor Kansas offers paid family leave, relying instead on the federal Family and Medical Leave Act, which provides only unpaid leave and applies only to employers with 50 or more employees. For women working in retail, food service, or for small employers, particularly common in rural areas, taking time off for frequent appointments can mean lost wages or job loss.
A 2019 study published in “Diabetes Spectrum” identified the demands of frequent medical appointments as a key obstacle to gestational diabetes care, especially for women facing financial constraints. Researchers found that women with lower socioeconomic status often perceived their health care providers’ expectations as unrealistic, given their work obligations and resources.
The Economic Burden
The financial strain of gestational diabetes extends beyond insurance coverage. Even women with insurance face substantial out-of-pocket costs. Glucose monitoring supplies, additional ultrasounds, specialist visits, and potential medications create expenses that accumulate throughout pregnancy.
Research on gestational diabetes care has found that diagnosis represents a substantial financial and time burden for women, according to a 2023 study published in the “Australian and New Zealand Journal of Obstetrics and Gynaecology.”Traditional care models required an average of 10 appointments for women managing the condition with diet alone and 15 appointments for those requiring insulin.
For uninsured women in Kansas’ coverage gap, these costs can be prohibitive. Even among insured women, copays and deductibles add up. Transportation expenses further compound the burden, particularly for rural women traveling long distances for care.
The Postpartum Gap
Both states have extended postpartum Medicaid coverage to 12 months. Kansas implemented the extension in 2022, and Missouri followed in November 2023, according to KFF. This represents meaningful progress, but it addresses only part of the problem.
The policy applies only to women who had Medicaid during pregnancy. Women in Kansas’ coverage gap still have no pathway to postpartum care, even though gestational diabetes signals elevated risk for future Type 2 diabetes. Research shows that 50% of women who experience gestational diabetes develop Type 2 diabetes within a decade, according to March of Dimes.
For many women, the story does not end with one pregnancy. They return to subsequent pregnancies carrying the metabolic consequences of inadequate care from the previous one, perpetuating a cycle of risk. Those accumulated risks do not stop with the mother.
The Intergenerational Cycle
The implications extend beyond individual pregnancies to future generations. Research published in Diabetes & Metabolism Journal describes how maternal hyperglycemia and resulting fetal hyperinsulinism lead to developmental and epigenetic preprogramming of cardiometabolic risk in offspring. This creates a cycle in which daughters born to mothers with gestational diabetes face a higher risk of developing the condition themselves.
Studies show that exposure to gestational diabetes in utero increases offspring risk of obesity by 54%, elevated body fat by 35%, and elevated waist circumference by 34% between ages 10 and 14. These effects persist into adolescence and adulthood, independent of postnatal environment.
Children of mothers with gestational diabetes also face increased risks of neuropsychiatric disease, ophthalmic problems, and cognitive impacts, according to research published in Frontiers in Clinical Diabetes and Healthcare. The effects are dose-dependent: the more severe the gestational diabetes, the greater the offspring’s risk.
“These data clearly show that we are not doing enough to support the health of the U.S. population, especially young women before and during pregnancy,” Shah said. “Public health and policy interventions should focus on helping all people access high-quality care and have the time and means to maintain healthful behaviors.”
What The Numbers Reveal
The steady year-over-year rise in gestational diabetes rates suggests that current interventions are insufficient. The issue is not a lack of awareness. It is a lack of structural support.
Coverage gaps mean that for many women, the first medical visit in years occurs only after pregnancy begins. Distance to care turns high-risk pregnancy management into a logistical challenge many families cannot sustain. The absence of paid leave forces women to choose between health and income.
Women need health insurance before pregnancy to identify and address metabolic risk factors. They need obstetric care within a reasonable distance of their homes. They need workplace policies that allow them to attend frequent medical appointments without sacrificing financial stability. They need postpartum care and monitoring, regardless of their insurance status during pregnancy.
In Missouri and Kansas, gaps across each of these areas converge to create conditions in which gestational diabetes rates continue to climb, year after year, with compounding consequences for women and their children.
What Needs to Happen Next?
Addressing gestational diabetes requires coordinated action. Policymakers must close insurance coverage gaps, protect rural maternity services, and ensure postpartum care does not end when pregnancy coverage expires. Employers must provide flexibility for frequent medical appointments without jeopardizing income or job security. Health systems must expand access to prenatal and diabetes care through community-based clinics, telehealth, and care coordination. Without accountability from each of these sectors, access to care will remain the limiting factor, not medical knowledge.
Calling state legislators, writing to governors’ offices, and supporting organizations working to expand Medicaid coverage, protect rural maternity care, and strengthen postpartum support are concrete steps toward improving access. Gestational diabetes is a medical condition, but the barriers to managing it are political, economic, and structural—and they will not change without public pressure.